Bioengineers at Johns Hopkins have succeeded in designing nanoparticles that are capable of safely and predictably infiltrating deep into the brain, thus paving the way to develop a drug-delivery system that can effectively treat brain cancer and other issues that impact the brain.
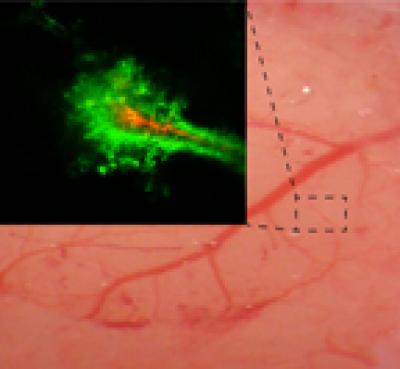 Real-time imaging of a rodent brain shows that nanoparticles coated with polyethylene-glycol (PEG) (green) penetrate farther within the brain than particles without the PEG coating (red). (credit: Elizabeth Nance, Graeme Woodworth, Kurt Sailor)
Real-time imaging of a rodent brain shows that nanoparticles coated with polyethylene-glycol (PEG) (green) penetrate farther within the brain than particles without the PEG coating (red). (credit: Elizabeth Nance, Graeme Woodworth, Kurt Sailor)
The researchers have described the testing of their nanoparticles in human tissue and live rodent brains in the Science Translational Medicine journal. Justin Hanes, Director of the Johns Hopkins Center for Nanomedicine, informed that the research team has discovered a method that allows the drug-embedded nanoparticles to penetrate deep into the brain by preventing them from binding to their surroundings.
It is very difficult to administer a chemotherapy dose effective enough to penetrate the tissue without affecting the surrounding healthy tissues. To overcome this problem, researchers fashioned nanoparticles to deliver drugs in tiny, constant volumes over a period of time. However, these nanoparticles have very low efficacy as they cannot penetrate deep into the tissue due to their tendency to attach to cells at the targeted site, stated Charles Eberhart, Johns Hopkins pathologist who contributed to this discovery.
Graeme Woodworth, Hopkins neurosurgeon, and Elizabeth Nance, a graduate student in chemical and biomolecular engineering at Hopkins, believed that it may be possible to improve drug penetration if the interaction between the drug-delivery nanoparticles and their surroundings is minimized.
For this purpose, Nance applied clinically proven poly(ethylene glycol) or PEG over different-sized nano-scale plastic beads. The researchers also suspected that the beads may become slippery when coated with a dense PEG layer. They then injected the beads that were labeled with glowing tags into human and rodent brain tissue. The glowing tags enabled the researchers to see the penetration of the beads into the tissue. What they discovered was the dense PEG coating enabled the penetration of even larger beads that have double the size of previously believed to be the optimum size possible for penetrating into the brain tissue, when compared to less densely coated beads and non-PEG-coated beads. They obtained the same results when they tested the coated beads carrying the chemotherapy medicine paclitaxel in rat brain tissue.
Nance stated that the researchers developed nanoparticles that are capable of carrying five folds more drug, release it for three folds as long and penetrate deeper into the brain. Woodworth commented that the next move is to explore the possibility of slowing down tumor recurrence or growth in rodents and upgrade the nanoparticles to deliver drugs for treating other brain diseases such as Parkinson's, Alzheimer's, traumatic brain injury, stroke and multiple sclerosis. The team is also exploring the possibility of intravenously administering its nanoparticles.