By pairing engineered nanoparticles with immune-based therapies, researchers are exploring new ways to turn resistant “cold” tumors into immune-active targets while improving drug delivery, reducing toxicity, and advancing the next generation of precision oncology.
Review: Nanotechnology Meets Immunotherapy: Crosstalks Against Cancer. Image Credit: CI Photos / Shutterstock
Cancer treatment is entering a new stage where nanotechnology is combined with the body’s immune system to target malignant cells more precisely. A recent review article in the journal Immunity, Inflammation and Disease explored how engineered nanoparticles (NPs) can overcome the limitations of currently approved cancer immunotherapies.
Researchers noted that currently approved immune checkpoint inhibitors benefit only 12% to 35% of patients, highlighting the urgent need for more effective strategies. The review highlights that nanomedicine can reprogram the tumor microenvironment (TME) and convert “cold” tumors into immunologically active ones, paving the way for more targeted therapies.
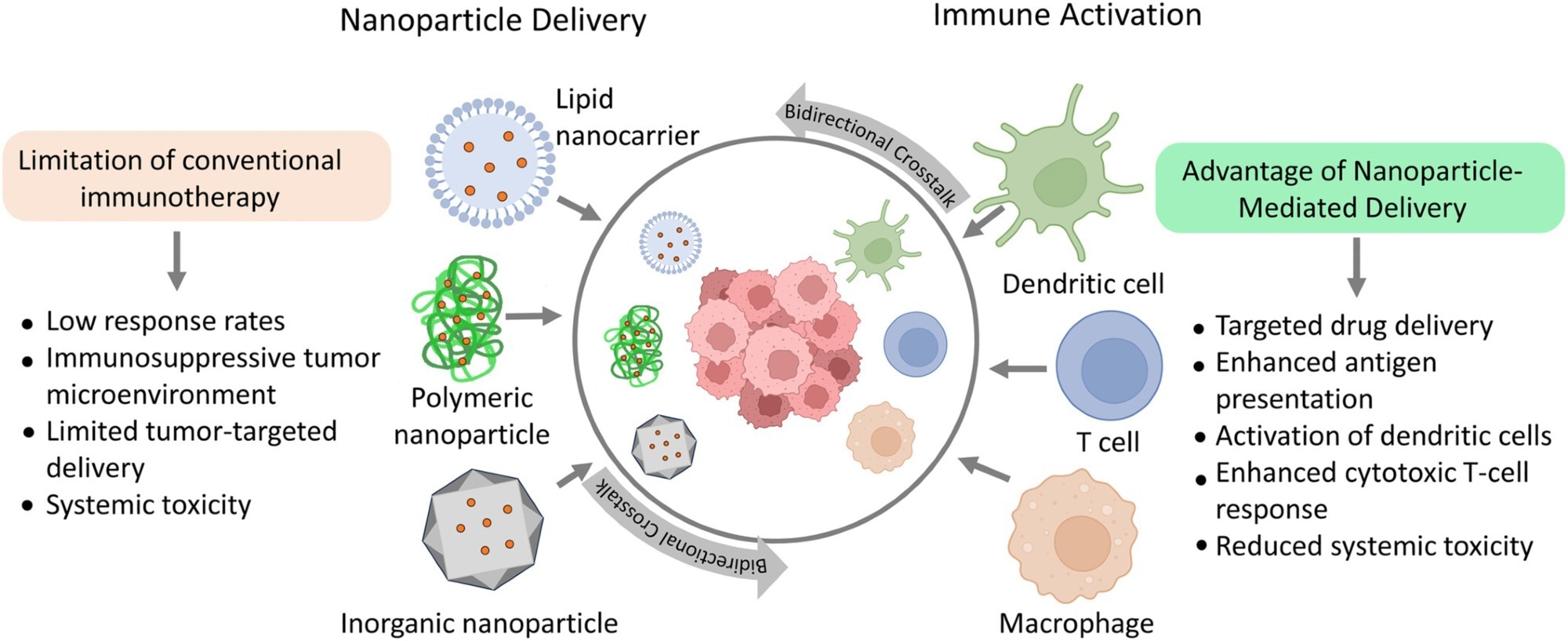
Schematic representation of the bidirectional crosstalk between nanoparticle-based platforms and immune cells in cancer immunotherapy. Different nanoplatforms, including inorganic (metallic), lipid-based, and polymeric nanoparticles, interact with key immune cells to enhance antigen presentation and stimulate antitumor immune responses within the tumor microenvironment.
Nanotechnology as an Enabling Platform in Oncology
The development of cancer therapy has progressed from traditional chemotherapy to more targeted immunotherapy approaches. However, conventional treatments often face challenges such as systemic toxicity, high recurrence rates, and the immunosuppressive TME. Nanotechnology addresses these challenges through the Enhanced Permeability and Retention (EPR) effect, in which leaky tumor blood vessels allow NPs, typically 10-100 nm in size, to accumulate selectively in cancerous tissues.
Using nanocarriers, scientists can improve the solubility of hydrophobic drugs and protect genetic materials, such as mRNA and siRNA, from degradation in the bloodstream. These nanoscale systems can also be modified with antibodies or peptides to cross biological barriers, including the blood-brain barrier. This targeted delivery approach helps reduce off-target effects while enhancing the availability of immunomodulatory therapies within tumors.
Designing Effective Nano-Immunotherapeutics
Researchers examined the physicochemical properties of various nanoplatforms, focusing on the structural design of materials, including metallic nanoparticles (MNPs), lipid-based nanoparticles, and polymeric systems such as PLGA (Poly(lactic-co-glycolic acid)). A major focus was on NP size optimization, as particles smaller than 10 nm are rapidly cleared through renal excretion. In comparison, those larger than 110 nm can become trapped in the lymphatic system.
The review also investigated “smart” nanocarriers with stimuli-responsive release mechanisms. These systems remain stable during circulation but release their therapeutic cargo when exposed to conditions within the TME, such as acidic pH or specific enzymes. Additionally, the authors explored biomimetic approaches, including cell membrane-coated NPs and artificial exosomes, which mimic natural biological structures to evade immune clearance and prolong circulation time.
Enhancing Immune Responses
The review highlights significant advancements in overcoming resistance in “cold” tumors. NP-mediated delivery of adjuvants, including TLR9 (Toll-Like Receptor 9) agonists such as CpG, can activate dendritic cells and stimulate the release of pro-inflammatory cytokines.
One important preclinical example involved synthetic high-density lipoprotein (sHDL) NPs. In mouse colon carcinoma models, these NPs, combined with anti-PD-1 (anti-Programmed Cell Death Protein 1) antibodies, achieved an 80% complete remission rate and increased cytotoxic T lymphocyte infiltration 7-fold, without the cardiotoxicity associated with free chemotherapeutic drugs.
Another key finding was the abscopal effect of metallic nanoparticles during photothermal therapy (PTT). Gold nanoshells and cuprous oxide nanoparticles absorbed specific wavelengths of light, generating localized heat that destroyed primary tumors. This process also released damage-associated molecular patterns (DAMPs) and tumor-associated antigens, helping the immune system recognize and attack distant metastatic tumors.
Clinical Applications and Translational Progress
Nanotechnology is increasingly applied in cancer immunotherapy. Nab-Paclitaxel (Abraxane), a 130 nm albumin-bound nanoparticle, improves tumor-targeted drug delivery by utilizing gp60 receptor-mediated transcytosis and the SPARC protein within the TME. In a phase II clinical trial, the combination of Nab-Paclitaxel with cyclophosphamide and trastuzumab achieved a 100% disease-free survival rate over 24 months in patients with HER2 (Human Epidermal Growth Factor Receptor 2)-positive breast cancer.
These platforms are also being explored for the development of cancer vaccines. DepoVax (DPX-0907) uses liposomal encapsulation to retain seven tumor epitopes and support long antigen presentation to the immune system in a dendritic-cell vaccine approach investigated in phase I trials for breast, ovarian, and prostate cancers. Additionally, nanodiscs are being developed to overcome multiple drug resistance (MDR) by bypassing P-glycoprotein efflux pumps that remove drugs from cancer cells. Other nanoparticle-based platforms and combinations are being investigated across multiple cancer types, including non-small cell lung cancer (NSCLC), breast cancer, advanced solid tumors, and pancreatic adenocarcinoma.
Adaptive and Personalized Therapies
In summary, the integration of nanotechnology and immunotherapy represents a significant shift in cancer treatment, with the potential to make some cancers more responsive to immune-based treatment. The review emphasizes that future advancements will depend heavily on theranostic platforms capable of simultaneously diagnosing, imaging, and treating tumors.
While challenges related to large-scale manufacturing, biosafety, long-term safety, targeting precision, batch variability, and regulatory approval remain, current research shows promising progress. Researchers also highlight the role of artificial intelligence (AI) and computational modeling in predicting patient-specific NP distribution within the body. By improving the interaction between engineered NPs and the immune system, future therapies may become more adaptive and personalized. Overall, nanotechnology provides a robust foundation for more precise and targeted immunotherapy.
Disclaimer: The views expressed here are those of the author expressed in their private capacity and do not necessarily represent the views of AZoM.com Limited T/A AZoNetwork the owner and operator of this website. This disclaimer forms part of the Terms and conditions of use of this website.